02 Mar Everybody Loves Data

post by Michael Galinsky and Suki Hawley
In the mid 18th century, before the world knew about germs, a Hungarian doctor named Ignaz Semmelweis worked in an Austrian hospital where the death rate of women giving birth was 13% because so many were dying of fever after birth. At a nearby midwifery, the death rate was only 2%. Semmelweis began looking into possible causes for such a large discrepancy. When his friend died of the same type of fever after cutting his finger in the morgue, Semmelweis instructed his students to wash their hands when moving from cadavers to the birthing room. The death rate dropped to 3%. However, Semmelweis’s observations conflicted with the established scientific and medical opinions of the time, and his ideas were rejected by the medical community. He didn’t offer any scientific evidence for these findings, and some doctors were offended at the suggestion that they should wash their hands. Eventually, he became so overwhelmed with rage that he ended up in an insane asylum where he died. Several years later when Joseph Lister discovered germs and used carbolic acid to kill them, he gave Semmelweis credit, “Without Semmelweis, my achievements would be nothing.”
Dr John Sarno didn’t end up in an insane asylum, but he was ridiculed and dismissed when in the 1970’s he discovered major flaws in how the medical system was dealing with back pain. Like Semmelweis, Sarno observed a problem, made a hypothesis about a possible solution, and tested it with his patients. When he found success, his colleagues dismissed his work. Also like Semmelweis, he published a book about his findings. While the book was hailed by patients for helping them recover when countless other methods failed, it too was ignored by his colleagues. Instead of letting rage destroy him or stop his work, he continued to treat patients and refine his theories. In 2012, he retired at the age of 89 with his work still unrecognized by his peers. Thankfully, the medical community is beginning to recognize its importance and validity, but he has not yet had his Joseph Lister moment of affirmation.
In the 1960’s, Dr John Sarno became frustrated when the standard care techniques he had been taught for treating back pain – things like bed rest, heat, traction, and physical therapy – didn’t seem to be helping his patients. Further, the explanations he was given for their pain, diagnoses like a pinched nerve or a herniated disc, often didn’t make anatomical sense. Frequently the position of the “impingement” or “herniation” didn’t correspond directly with where the pain was occurring. More often than not – even if it did make some anatomical sense – the patient would also have pain in other locations that couldn’t be explained by the “physical abnormality” that was pinpointed as the cause. He examined his patients’ charts and found that over 80% of them had a history of two or more illnesses that were commonly thought to have a mind body component – things like ulcers, migraines, colitis, eczema, and anxiety. Upon speaking with his patients, he quickly realized that they tended to be what he termed “goodists” – perfectionists or “people pleasers” – who put themselves under inordinate pressure to put personal achievement or other people’s needs above their own needs. He postulated that this impulse was borne out of behavior learned in early childhood, of suppressing their emotions (often unconsciously) in order to avoid conflict with a parent or sibling. When he pointed out the connection between this tendency combined with life stressors and their back pain, awareness of the connection often led to the pain resolving itself. While he couldn’t find much scientific data that supported either the physical diagnosis of the cause of the pain nor its treatment, he did find a number of studies that corroborated his hunch that the issue might be psychosomatic. When we interviewed Dr Sarno in 2004 he explained:
Eighty eight percent of the people I was seeing had histories of 1 to 4 of these other mind body disorders. And then all of a sudden I said ‘Hey, maybe this is a mind body disorder. too.’ And then I came across some of the articles that had been published by these doctors in the ‘30’s and ‘40’s. And they said rage was the major factor. I began to put it to them, and of course many patients said, ‘No that’s ridiculous,’ but some of them said, ‘Yeah, maybe…’ – and those are the patients who got better. Again, we can put this very broadly: that we all generate feelings in the unconscious mind of which we are totally unaware as a result of our life experiences which begin in childhood.
After studying his patients’ progress and perfecting his technique for more than a decade, he published a book aimed at patients called “Mind Over Back Pain“. In it, he predicted that if the medical community continued to make the wrong diagnosis by focusing solely on physical symptoms rather than the true cause which he argued had an emotional basis, there would be an epidemic of pain. Because Sarno did not back up his theories with randomized controlled trials (RCT), which are seen as the “gold standard” of scientific data, his colleagues easily ignored him and his theories (when his work was discussed on ABC News’s 20/20 in 1999, a medical colleague at his hospital invidiously compared his mind body ideas to “swinging a cat around your head three times”). Dr. Sarno countered that emotional factors are not something that can be controlled for or studied in a laboratory in the same way that you can study factors like diet or whether or not a particular drug affects cells in a specific manner:
How do you prove the existence of unconscious emotions? How do you demonstrate them? How do you quantitate them? You can’t. You can only use close honest observation, tried methods of treatment and see the ones that work and the ones that don’t and so on. But as far as they’re concerned, if you can’t put numbers to it then it doesn’t exist.
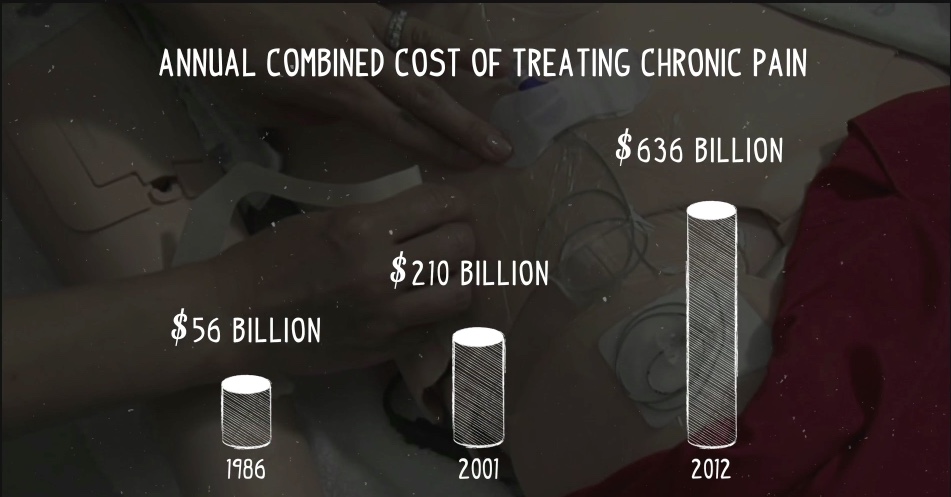
He continued to focus on treating his patients and publishing a series of books written for patients and practitioners alike. Meanwhile, pain syndromes grew at such an enormous rate that the cost of dealing with them now dwarfs almost all other medical costs – including heart disease, cancer, and diabetes combined.
Gina Kolata and The New York Times
In 2012, Dr Sarno was forced to retire because his office at NYU was being torn down to build a modern laser spine clinic. While his colleagues continued to argue that only the “gold standard” of randomized controlled trials of his methods would convince them that he was right, they ignored the fact that these same types of trials were not supporting the work that they did. RCT’s testing the validity of things like a correlation between disc abnormalities and pain continuously failed to prove such a correlation. In fact, as Gina Kolata wrote in a NY Times article last fall “Why ‘Useless’ Surgery Is Still Popular”, the evidence for back surgery and MRI’s continues to invalidate their use, but they persist nonetheless:
It looks as if the onus is on patients to ask what evidence, if any, shows that surgery is better than other options.
Take what happened with spinal fusion, an operation that welds together adjacent vertebrae to relieve back pain from worn-out discs. Unlike most operations, it actually was tested in four clinical trials. The conclusion: Surgery was no better than alternative nonsurgical treatments, like supervised exercise and therapy to help patients deal with their fear of back pain. In both groups, the pain usually diminished or went away.
The studies were completed by the early 2000s and should have been enough to greatly limit or stop the surgery, says Dr. Richard Deyo, professor of evidence-based medicine at the Oregon Health and Sciences University. But that did not happen, according to a recent report. Instead, spinal fusion rates increased — the clinical trials had little effect.
In 2004, Ms. Kolata began by publishing an article about the futility of treating back pain, (“With Costs Rising, Treating Back Pain Often Seems Futile”).
“Yet for all the costs, for all the hours spent in doctors’ offices and operating suites, for all the massage therapy and acupuncture and spinal manipulations, study after study is leading medical experts to ask what, if anything, is doing any good.
A variety of studies have suggested that in 85 percent of cases it is impossible to say why a person’s back hurts, said Dr. Richard Deyo, a professor of medicine and health services at the University of Washington. And most of the time, the pain goes away with or without medical treatment.”
In 2006, she reported on another medical report, “Study Questions Need to Operate on Disk Injuries”. Then in 2009, her colleague Tara Parker-Pope wrote an article entitled, “Scans for Back Pain Ineffective”. Ms Kolata has been reporting about results confirming previous results time and again, yet practice doesn’t change. Instead, the use of surgery, steroid shots, and opioid prescriptions continue to grow, and Dr. Sarno continues to be ignored despite the growing body of evidence supporting his assertion about the futility of standard care.
When we read Kolata’s first article in 2004, we had just started to make a film about Dr. Sarno called All the Rage. We asked if we could interview her about the article, but she said she didn’t want to become part of the story. At the time we found that not many people wanted to be associated with Dr Sarno because he was such an outlier. In fact, we had so much difficulty getting people to talk about him, or fund the film, that we had to put it on hold. When we came back to it 7 years later, things had shifted considerably. Other doctors in different fields had discovered how powerful the mind body connection is, and published their own books to get the message out. Dr. David Clarke’s book “They Can’t Find Anything Wrong” focused on gut issues and Gabor Mate’s book “When the Body Says No” zeroed in on how the repression of emotions is connected to auto immune issues. When Mate recognized the possible mind body connection, he went to see if there was any research supporting this idea and found a great deal. However, for the most part, no one was paying attention to it because it ran counter to the accepted ideas of the day.
American College of Physicians
In February of 2017, the American College of Physicians issued a new set of guidelines that seem to vindicate Dr. Sarno’s primary contention that standard care wasn’t based on solid data. However, they only hint at the emotional cause of the problem. The report instructs physicians to avoid diagnostic and treatment interventions which can be costly and dangerous because the data doesn not support their use. These include doing MRI’s (because even when herniations are present, data show there is no solid causal correlation between herniation and pain), opioids, and anti-inflammatories like Tylenol.* Instead, the report suggests yoga, mindfulness, and acupuncture, tacitly recognizing that a mind body connection is at play. Unfortunately, this report is too little and too late, because Dr. Sarno’s astute prediction about an epidemic of pain has become horribly true. As stated above, chronic pain dwarfs almost all other medical expenses combined. It is now a trillion dollar per year problem. Unfortunately, it is hard to believe even with these new guidelines that standard practice will change with any real urgency or speed. The guidelines were trumpeted by major news media but quickly drowned out by a flurry of political chaos. How can this be?
The New Yorker
Elisabeth Kolbert wrote about this issue in the New Yorker on Feb 27th in an article titled, “Why Facts Don’t Change Our Minds”. In the article, she chronicles several new books that zero in on this idea. She begins the article with a discussion of subjects’ reactions to the fact that they had been told false facts during studies done at Stanford in the 1970’s.
Even after the evidence “for their beliefs has been totally refuted, people fail to make appropriate revisions in those beliefs,” the researchers noted. In this case, the failure was “particularly impressive,” since two data points would never have been enough information to generalize from.
The Stanford studies became famous. Coming from a group of academics in the 1970’s, the contention that people can’t think straight was shocking. It isn’t any longer. Thousands of subsequent experiments have confirmed (and elaborated on) this finding. As everyone who’s followed the research — or even occasionally picked up a copy of Psychology Today — knows, any graduate student with a clipboard can demonstrate that reasonable-seeming people are often totally irrational. Rarely has this insight seemed more relevant than it does right now. Still, an essential puzzle remains: How did we come to be this way?
To make a long story short, many researchers believe that we developed this pattern because we are social creatures. Learning to cooperate, and giving deference to power, are adaptations used to grease the cogs of social interaction. While this pattern of behavior may help in small groups settings, it seems to be problematic when faced with the threat of fascist authoritarianism, or entrenched systems in which those in power accrue benefits from their position in terms of compensation and respect – like doctors within our current medical system.
As a culture, we place a great deal of faith in data to guide us as we make decisions and plans. People with degrees and higher levels of education are treated with deference and respect in large part because they both create data sets as well as know how to use, and take advantage of, data. Having been taught that the rigorous training that doctors and scientists receive gives them great insight and knowledge, we often find it very difficult to question them. Because of our respect for doctors and scientists, we also expect them to be able to answer difficult and complex questions about our health; and that they be able to offer solutions that will cure our ills. In fact, data make it clear that when we leave a doctor’s office without a prescription we have a much less favorable view of our visit. Even though doctors are often presented with situations that don’t offer a clear solution, patients are frustrated if they aren’t given one.
A couple of years ago I told my cousin that the only reason that doctors prescribe antibiotics for strep throat is a small study that was done on an army base in the 1950’s. In this study, it was found that among 100 soldiers with strep throat, investigators found 2% of patients in the control group who did not get antibiotics developed Rheumatic Fever. Among those who did take penicillin, 1% got Rheumatic Fever. Based on that single study, which indicated a 1% decrease in Rheumatic Fever, it was recommended that antibiotics be given. Unfortunately, at the time there was not an understanding that there might be adverse effects from the use of antibiotics, like anti-biotic resistance, or an effect on our gut biomes. My cousin, who is a history of science professor, refused to believe me because it was clear to him that this wasn’t a solid enough foundation for the recommendation. After three hours of searching Lexis Nexis, he finally had to concede: the only thing he could find was the study I cited. The point here is that much of what we blindly accept as being built on solid science is not so solid after all. We want to believe that doctors have a factual foundation from which they base their decisions, when in reality they are largely doing what the have been taught even though much of that is not based on solid evidence.
It is human nature to desire clarity. We place great value in data that can be used to tell a clear and simple story. As filmmakers, my partners and I struggle with this reality. We tend to tell complex tales in which there isn’t a clear hero or villain, and this can make it difficult for us to reach an audience that doesn’t want to struggle with complexity. There is a great deal of pressure on us to do what is expected, and because we don’t, we find that it is hard to get people in positions of power to accept our work. The same is true for scientists and doctors. They are under enormous pressure to do the kind of studies that will yield clear data, even when that clarity makes the data less useful in real world terms. This desire for clarity carries over to the media which often jumps on reports and studies that seem to have clear and catchy narratives – even when the studies themselves are less clear. Every few years the story changes: “fat is bad” is followed by “fat is good”, or “sugar is safe” is followed by “sugar is a killer”. In reality there are complex forces at play in why and how food or medicine affects our bodies and the studies are often much less clear than they are purported to be. Despite naysayers, the overriding paradigm stays in place until either a charismatic authority highlights the problem (currently this can be seen with Robert Lustig and the sugar debate) or the evidence becomes so clearcut that the major institutions call for a change in practice (in the Case of the American College of Physicians’ guidelines). Both of these situations involve the participation of the media to broadcast the need for a change.
ProPublica and The Atlantic
I began this piece with a discussion about Dr. John Sarno and back pain, but the problem of ignoring data which don’t conform to what we expect, doesn’t just exist in relation to pain. A few weeks ago I posted this piece about Robert Lustig’s efforts to sound the alarm on the hazardous effects of sugar. After Lusting published research connecting sugar to a myriad of health issues he was asked whether he had based his work on John Yudkin’s previous studies. Unfortunately, he had never even heard of Yudkin because his research had been overshadowed by a competing theory, that animal fat was causing heart disease. We want to believe that the scientific system’s checks and balances make sure that useful data is easily accesible. It’s not true. Unseen forces often shape the narrative. This week ProPublica and The Atlantic collaborated on an in-depth look at how the medical community has ignored vast swaths of data – even when they relate to dangerous procedures showing no evidence of a clear benefit but great risk of life-threatening harm, “When Evidence Says No, But Doctors Say Yes”. The article points out that despite reams of data making clear that stents do not prevent heart attacks when used on people who are stable, their use has not declined. The subhead of David Epstein’s article could have been lifted from the American College of Physicians guidelines (or one of Gina Kolata’s Times articles):
Years after research contradicts common practices, patients continue to demand them and doctors continue to deliver. The result is an epidemic of unnecessary and unhelpful treatment.
The article goes on to point out a myriad of examples whereby inconclusive evidence leads to a change in practice, like surgically implanting stents into stable heart patients with constricted arteries, or taking beta blockers to prevent heart attacks in people with high blood pressure. When evidence emerges that makes it clear that these techniques don’t reduce heart attacks or death – and in the case of the surgical implant of stents, the evidence underscores greater risk involved – the evidence doesn’t affect practice. The point is, these situations are complex. Medical facts get mixed up with impulses better studied by social psychologists. In the end, we make decisions in highly unreasonable manners. That’s fine. We just need to recognize that fact rather than pretend that data is pure, clean, and provides answers that shouldn’t be questioned. At this point it should be clear that there are problems with the way that data gets produced, interpreted, and implemented. This is not to say that the data is always manipulated with nefarious intentions, but instead that when we exist inside a system, we are often blind to the problems that the system contains- especially if our livelihood depends on that system functioning as it does.
Afterword – The Film
Our film All the Rage is largely about Dr Sarno and his ideas. It is also a personal story about pain and like Dr. Sarno, we have met resistance to the basic premise of the film, that our minds and bodies are intimately connected. However, those who are open to the ideas presented have found it profoundly helpful. I’ll close with a few notes we got this week from therapists and from other filmmakers who recently viewed the film.
“Michael — I LOVE LOVE LOVE the documentary. I have one patient whose life has been dramatically changed as a result of Sarno’s theory and psychotherapy.”
-LM LCSW
“I just finished watching the movie and I’m crying. It is a profound gift, a profound message and a profound hope. It takes the mind-body concept another step closer to becoming the mainstream approach to not only pain, but to all things that happen in the body. Cellular memory is real. I cannot wait to share this movie. Please tell me it will soon be released. It is so valuable and it is certain to have a deep impact on the public audience. You are changing the world. I am so grateful to have found you and Dr. Sarno. I bow to you,
– DS therapist
“Congrats. I found the film to be informative and sensitively done. It accessed my emotions. It emphasized the 2 important ideas : the significance of the mind/body connection and that our pain is distracting us from dealing with our emotional issues. This is a critical understanding and I’m sure difficult for many people to get.”
-SK LCSW
“I just watched your film tonight. It was so eyeopening and really well done. I think you did an excellent job crafting a compelling story around a subject without a clearcut storyline. I also commend you for putting yourself in the film in such a vulnerable way. Everything in the film really resonated with what by dad has been dealing with for years. I wish he had read Dr. Sarno’s books before he had his laminectomy, which has since proved to be completely unsuccessful. With your permission, I would love to share your film with my parents. I think it could really help my dad. He’s a total skeptic about this kind of stuff but I think if he hears and sees so many people’s testimonies, it might actually have an impact on him.”
– JS Filmmaker
“Thank you so much for sharing your film ALL THE RAGE with me. It was deeply moving and mesmerizing but beyond that… your story and Dr. Sarno’s work really hit me hard. I had to watch the film twice and let it sink in me. It made me rethink my ailments, depression and how I’ve been dealing with my childhood trauma in my art and in life. So eye opening!!! My partner happened to have the doctor’s book, so I started reading it. I found myself debating with your narration and with myself throughout the film. I hope so many people get to watch this film and have AHA moments, as I did. THANK YOU!”
– HP Filmmaker
*I have edited this post after it was published. It previously included steroid shots and surgery as modalities that the ACP suggested avoiding. This is not explicitly stated- so it was removed.
Mauricio Bustamante
Posted at 20:12h, 03 MarchLong overdue study of this problem.
George Entenman
Posted at 20:09h, 30 MarchWhat you’ve experienced in the medical world reminds me of Daniel Dinnett’s attempts to get philosophers to think more scientifically (The New Yorker – http://www.newyorker.com/magazine/2017/03/27/daniel-dennetts-science-of-the-soul). (I don’t really think that your article is trying to do the opposite – I interpret it as wanting science to pay attention to new types of data).
Anyway I thought of you when I read this wonderful sentence: “Arguments, Dinnett found, rarely shift intuitions; it’s through stories that we revise our sense of what’s natural”.
Patrick
Posted at 06:01h, 07 AprilEyes opening post.